Estrogen does a lot more than regulate periods. It helps shape your sleep, mood, skin, sex drive, bones, and even how much energy you have day to day.
When estrogen drops, the signs can show up in ways that feel unrelated at first. You might notice night sweats, mood swings, vaginal dryness, dry skin, brain fog, or a dip in desire, and some people also deal with fatigue, headaches, and irregular periods. If you’re trying to make sense of several small changes at once, foods that balance estrogen naturally can be a useful place to start while you sort out what’s going on.
Still, these symptoms can overlap with stress, thyroid problems, perimenopause, poor sleep, and other health issues, so this guide is for awareness, not self-diagnosis. The goal is to help you notice patterns early and understand when it makes sense to talk with a clinician.
Here are the 15 signs of low estrogen to watch for, and what they may mean for your body.
What low estrogen means and why it happens
Low estrogen means your body is making less estrogen than it needs to keep several systems running smoothly. This hormone helps regulate the menstrual cycle, supports bone strength, keeps vaginal tissue moist and flexible, affects skin and brain function, and helps the body control temperature.
When estrogen drops, the effects can show up in more than one place at once. That is why low estrogen can cause changes in periods, sex drive, sleep, mood, and hot flashes. It can also make bones more fragile over time, which matters even if you do not feel any symptoms right away.
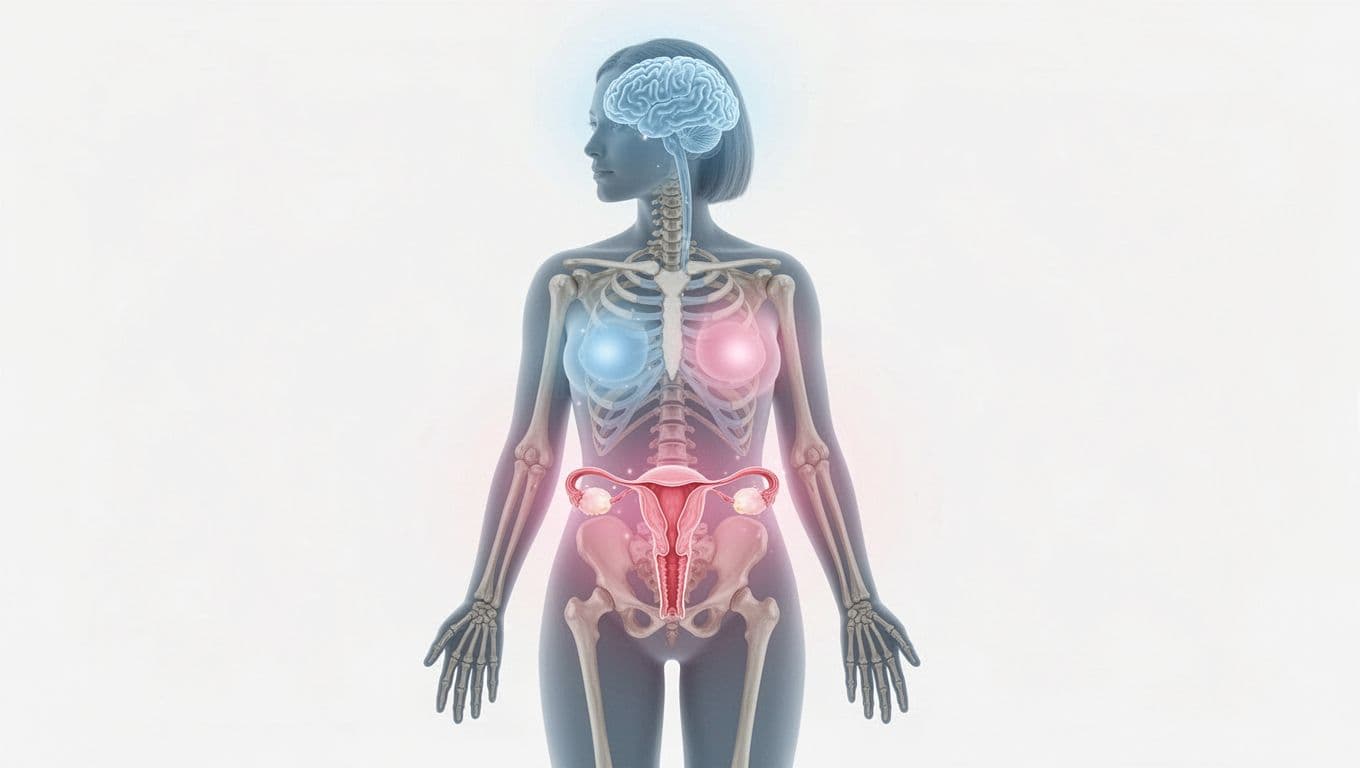
Why estrogen matters in the body
Estrogen helps the lining of the uterus build and shed on schedule during the menstrual cycle. It also supports healthy vaginal tissue, which is why low levels can lead to dryness or discomfort during sex.
Bones rely on estrogen too. When levels stay low, the body can lose bone mass faster. Skin may also feel drier or thinner, and the brain can feel the shift through mood changes, brain fog, or sleep problems.
Common reasons estrogen drops
The most common reason is perimenopause, the years before menopause when hormone levels rise and fall. Menopause follows after periods stop for 12 straight months.
Other causes include:
- Premature ovarian insufficiency, when the ovaries stop working normally before age 40
- Very low body weight or eating disorders, which can reduce hormone production
- Intense exercise paired with too little fuel
- Certain medical treatments, such as chemotherapy, radiation, or ovary removal
- Problems with the ovaries or pituitary gland, which can interrupt hormone signals
For a broader look at hormone-related symptoms, high cortisol signs can also overlap with some low-estrogen complaints, which is one reason patterns matter more than any single symptom.
The most common body changes linked to low estrogen
Low estrogen often shows up in the body before anyone connects the dots. Some changes are sudden and obvious, while others build slowly and feel easy to blame on stress, age, or poor sleep.
The signs below are the ones readers usually notice first. Some affect the reproductive system, while others show up in the skin, hair, joints, or daily comfort. Together, they can point to a hormone shift that deserves attention.
Hot flashes and night sweats can be early clues

Hot flashes usually feel like a sudden wave of heat that rises through the face, neck, and chest. Your skin may flush, your heart may race, and you may start sweating fast.
Night sweats are the same kind of heat surge, but they hit during sleep. They can soak your sheets, wake you up, and leave you tired the next day. When sleep keeps getting broken, even simple tasks can feel harder.
These symptoms happen because estrogen helps the brain regulate body temperature. When estrogen drops, that thermostat can become too sensitive.
If you want a deeper medical overview, Cleveland Clinic’s low estrogen guide gives a clear breakdown of how these symptoms show up.
Periods that change, skip, or stop may point to hormone shifts
Estrogen helps control the menstrual cycle, so changes in your period often show up early. Your cycle may become lighter, heavier, shorter, longer, or harder to predict. Some periods may simply not show up at all.
These changes can happen in perimenopause, but they can also come from other health issues. Pregnancy, thyroid problems, stress, weight changes, and certain medications can all affect your cycle too.
A changing period is a clue, not a diagnosis.
If your cycles are suddenly different for several months in a row, that pattern matters. It can point to hormone shifts, but it also deserves a proper checkup.
Vaginal dryness and painful sex often come from thinning tissues
Low estrogen can make vaginal tissue thinner, drier, and less flexible. That often means less natural lubrication, more friction, and pain during sex. Some people also notice burning, itching, or a feeling that things are just more sensitive than before.
This is where vaginal dryness and thinning tissue can become part of the bigger picture. These changes can also raise the risk of irritation, urinary discomfort, and more frequent urinary tract infections.
Dry skin, thinning hair, and joint aches can also be part of the picture
Estrogen helps skin hold moisture and stay elastic. When levels fall, skin may feel dry, rough, itchy, or more fragile than usual. Hair can also shed more or look thinner, especially along the part line or crown.
Joint aches are another common clue. You may feel stiffness in the morning, soreness after activity, or more overall body tenderness.
A few body changes often travel together:
- Dry skin can feel tight, flaky, or more sensitive.
- Thinning hair may show up as more shedding or less volume.
- Joint pain may feel like stiffness, aching, or reduced flexibility.
Low sex drive can show up here too, since hormone shifts can affect both desire and comfort.
How low estrogen can affect your mood, sleep, and thinking
Low estrogen does more than affect periods or vaginal comfort. It can also change how you feel, how well you rest, and how clearly you think. Those shifts can look a lot like stress, burnout, or just “getting older,” which is why they often get missed.
The brain is sensitive to hormone changes. Estrogen helps support mood-related brain chemicals, sleep patterns, and memory. When levels drop, the effect can feel like a shaky filter over everyday life, where small problems feel bigger and your mind has a harder time keeping up.
Mood swings, anxiety, and feeling more emotional than usual

When estrogen changes, serotonin and other brain chemicals can shift too. That can show up as sudden mood swings, more worry, irritability, or tears that come on faster than usual. You may feel fine one minute, then overwhelmed the next.
This can be especially confusing if you do not usually struggle with anxiety or low mood. The change may feel small at first, but it can chip away at your patience and confidence over time. In some people, estrogen swings also make stress feel louder than it really is.
Research also points to changes in how the brain handles emotion during perimenopause. That is one reason mood symptoms can appear even when life circumstances have not changed much. If emotional ups and downs feel new, a hormone shift may be part of the picture.
Trouble sleeping and constant fatigue can feed each other
Low estrogen can disrupt sleep in more than one way. Night sweats may wake you up, insomnia can make it hard to fall back asleep, and restless sleep can leave you feeling like you never fully recharged.
That lack of sleep does not stay in the bedroom. It can lead to daytime exhaustion, lower focus, and shorter patience with everyone around you. A bad night can also make the next day feel emotionally sharper, so small annoyances hit harder.
If your sleep has been off for weeks, the cycle can snowball. Poor sleep raises stress, stress makes sleep worse, and both can leave you drained. For more on that cycle, see how sleep loss affects fatigue.
Brain fog can make it harder to concentrate and remember things

Brain fog often feels like mental drag. You may lose track of words, forget simple tasks, walk into a room and wonder why you went there, or feel slower than usual when you try to think through a problem.
This happens because estrogen supports attention, memory, and other brain functions. When levels drop, you might notice it in small but frustrating ways, especially when you’re tired. A good night’s sleep helps, but if sleep is already broken, concentration gets even harder.
If this sounds familiar, brain reboot tips can help you understand the role rest plays in mental clarity.
When mood, sleep, and memory all change at once, hormone shifts are one possible reason to consider.
These symptoms do not always mean low estrogen, but they do deserve attention, especially when they cluster together.
Signs that low estrogen may be affecting your urinary and bone health
Low estrogen does not only change how you feel day to day. It can also affect parts of the body that are easy to overlook at first, especially the bladder and the bones. Those changes may start small, but they can build over time.
When estrogen drops, tissues in the urinary tract can become thinner and drier. Bones can also lose strength faster than they should, which raises the risk of osteoporosis later on. If you notice repeated bladder problems or ongoing bone pain, do not brush them off.
More bladder irritation or UTIs can happen when tissues dry out

Estrogen helps keep the bladder, urethra, and nearby tissues healthy and flexible. When levels fall, those tissues can dry out and become more sensitive, which may lead to urinary urgency, burning, pressure, leakage, or a feeling that you always need to go.
This can also raise the chance of recurrent UTIs, since the urinary tract has less protection and bacteria can grow more easily. A Cleveland Clinic overview of low estrogen symptoms notes that urgency, incontinence, and UTIs often show up together during the menopause transition.
If you keep getting bladder symptoms, pay attention to the pattern. One infection can happen for many reasons, but repeated irritation deserves a closer look.
Bone loss is a long-term risk that should not be missed

Estrogen helps slow bone breakdown, so lower levels can speed up bone loss. Over time, that can weaken bones and raise the risk of osteoporosis, even before you feel a clear problem.
Many people expect bone trouble to come with a dramatic warning sign, but it often starts quietly. You may notice back pain, loss of height, or a fracture after a small fall. That is why prevention matters early, not after damage is already done.
The Mayo Clinic’s guide to perimenopause symptoms also points out that estrogen loss can speed bone thinning. If bone pain, repeated fractures, or urinary symptoms keep showing up, they deserve medical attention, not guesswork.
When these symptoms may be something else
Low estrogen can explain a lot, but it’s not the only reason these changes happen. Hot flashes, fatigue, mood swings, dry skin, brain fog, and irregular periods can also show up with other health problems, so the pattern matters as much as the symptom itself.
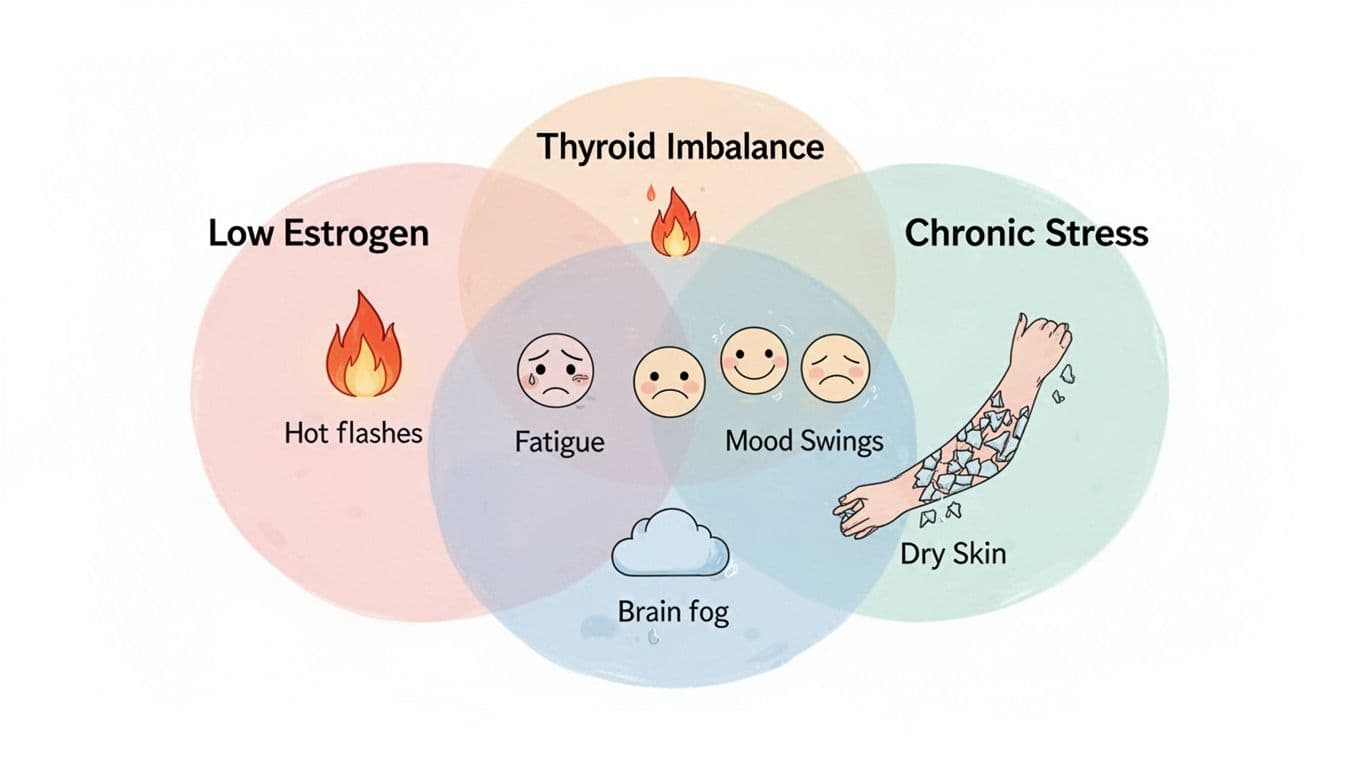
Thyroid problems can look very similar
Thyroid disorders, especially hypothyroidism, can cause fatigue, weight changes, dry skin, mood shifts, and brain fog. Some people also notice temperature changes and irregular periods, which makes it easy to confuse with low estrogen.
That overlap is one reason blood tests matter. If symptoms keep building, a thyroid check can help separate one issue from another.
Stress, anemia, and depression can blur the picture
Chronic stress can throw off sleep, energy, mood, and hormones. Anemia can leave you drained, foggy, and weak. Depression can also show up as low energy, sleep trouble, poor focus, and less interest in sex.
Medication side effects can do the same thing. Hormonal birth control, steroids, antidepressants, and some cancer treatments can all change how your body feels.
Pregnancy, postpartum changes, and other hormone issues matter too
Pregnancy and the months after birth can cause big hormone shifts, especially if you’re breastfeeding. Other hormone issues, like premature ovarian insufficiency or pituitary problems, can also cause symptoms that look like low estrogen.
The clue is often the pattern, not one symptom alone.
If several symptoms started around the same time, or they line up with cycle changes, that matters. If they came on during a stressful stretch, after a new medication, or alongside heavy bleeding, those details matter too. Paying attention to timing, triggers, and how many symptoms are happening together can help you and your clinician narrow it down faster.
How doctors check for low estrogen and what treatment may look like
If your symptoms keep pointing toward low estrogen, the next step is a clinical checkup, not guesswork. Doctors usually start by looking at the full pattern, then decide whether testing can help narrow the cause.

What to expect at a doctor visit
The visit often begins with questions about your cycle, sleep, mood, hot flashes, vaginal dryness, sex drive, and bladder changes. A doctor may also ask about age, recent weight changes, exercise habits, stress, pregnancy risk, and any new medicines, since all of these can affect hormones.
Next comes a review of your medical history. That matters because low estrogen can happen for different reasons, and treatment changes based on the cause. For example, symptoms in a woman in her 40s may point to perimenopause, while symptoms before age 40 may raise concern for premature ovarian insufficiency.
Blood tests can help in some cases. Doctors may check estradiol, FSH, and LH to look at how the ovaries and brain are communicating. Results are more useful when they match the symptom pattern, because hormone levels rise and fall during the cycle. In many women over 45 with typical menopausal symptoms, blood tests are not always needed first, which is why symptom review matters so much. The Cleveland Clinic’s low estrogen overview gives a clear summary of the common tests used.
Testing can look different based on your age, cycle stage, and whether you are already in menopause.
Treatment options may include hormones, non-hormone medicine, and lifestyle support
Treatment depends on your symptoms, age, medical history, and whether you still have a uterus. For many people, hormone therapy is the most effective option for hot flashes, night sweats, and bone protection. If symptoms are mainly vaginal, doctors often use vaginal estrogen, which targets dryness and pain with less whole-body exposure.
When hormone therapy is not a good fit, non-hormone medicines may help with hot flashes or mood symptoms. Lifestyle support also matters. Better sleep, regular exercise, a steady diet, and simple vaginal lubricants can ease symptoms and make daily life more comfortable.
The right plan is usually the one that matches the person, not just the lab result. A treatment that helps one woman may not be the best choice for another, which is why your health history guides the decision.
Conclusion
Low estrogen can touch far more than your cycle. It can affect periods, sleep, mood, sex drive, skin, hair, urinary comfort, and long-term bone health.
One symptom on its own does not prove low estrogen. However, when several signs show up together, especially with cycle changes or new vaginal dryness, hot flashes, or brain fog, it is worth paying attention.
Getting checked can bring real relief and a clearer plan. With the right care, you can ease symptoms now and help protect your health over time.
Save the pin for later

- Why Fiber Is the Standard for Your Home Internet - 16/05/2026
- How to Bounce Back From a Setback (A Step-by-Step Guide) - 16/05/2026
- 12 Practical Ways to Rebuild Your Confidence After Failure - 16/05/2026
