Fatty liver, now often called MASLD, happens when excess fat builds up in the liver, and it’s showing up more often in teens, people in their 20s, and people in their 30s. That matters because the condition can stay quiet for years, so many people miss it until lab work or scans catch a problem. A recent NBC Nightly News segment on the trend is here: Study Shows More Young People Dying From Liver Disease.
Poor diet, less movement, weight gain, and insulin resistance are pushing risk higher, but added sugar plays a big part too, which is why cutting back on sugar can matter. The next section breaks down the biggest reasons this is happening, the signs people often miss, and why acting early makes a real difference.
What fatty liver means, and why doctors are worried
Fatty liver means too much fat has built up in the liver. At first, that may sound minor, but the liver is a busy organ, and extra fat can make it work less well over time. If the buildup keeps going, it can lead to inflammation, then scarring, and in more advanced cases, lasting liver damage.
You may also see the newer term MASLD, which stands for metabolic dysfunction-associated steatotic liver disease. The name changed because doctors now understand that this condition is tied to metabolic problems, like insulin resistance, excess body fat, and poor blood sugar control, not just weight alone. That’s one reason steady blood sugar habits matter so much. When fatty liver is caught early, it can often be reversed before serious damage starts.
How a healthy liver becomes overloaded with fat
A healthy liver helps process nutrients, store energy, and clear waste from the blood. When you take in more energy than your body needs, especially from added sugar, refined carbs, and excess calories, the liver can start turning that surplus into fat. Over time, those fat droplets collect inside liver cells and crowd them like boxes piling up in a small room.
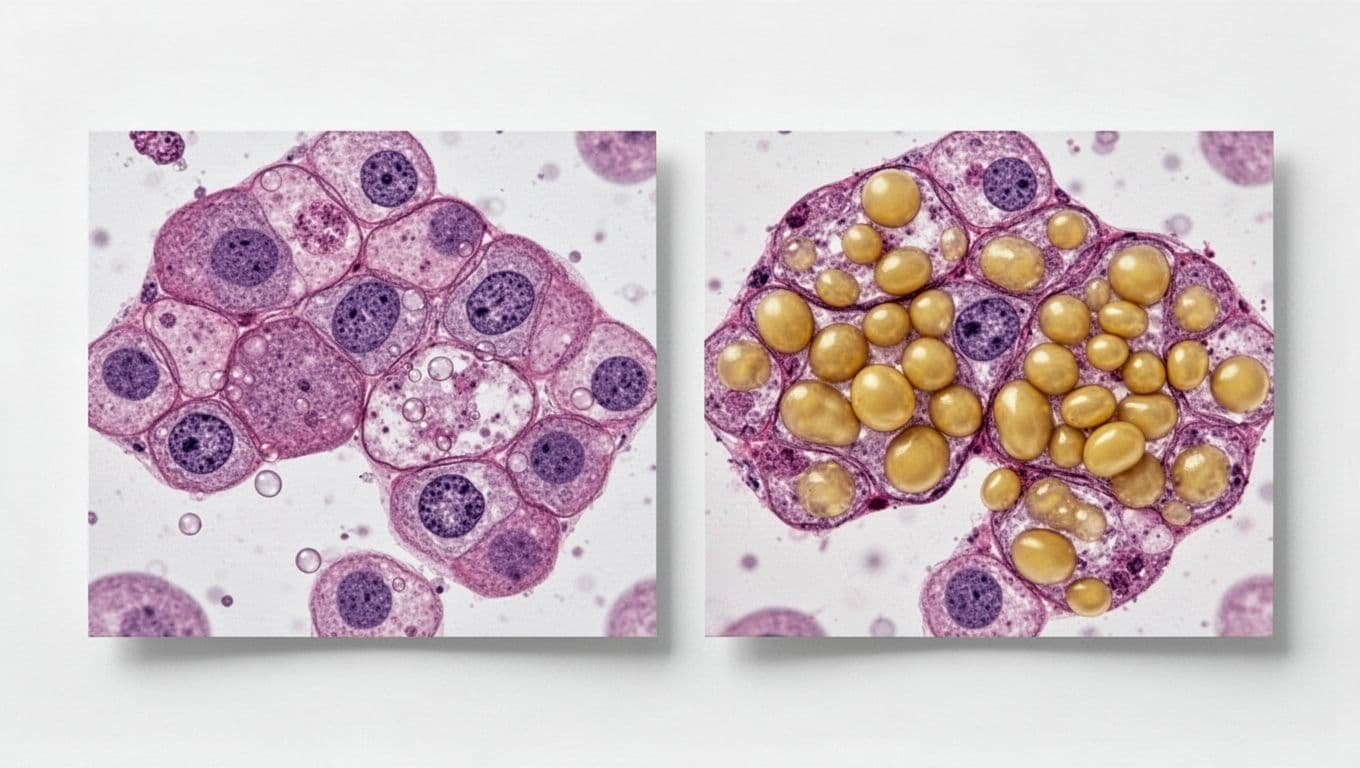
As fat builds up, the liver cannot do its job as smoothly. That extra load can interfere with normal function and, in some people, trigger irritation in the tissue. If the process continues, simple fatty liver can turn into a more serious form with inflammation and scarring.
The good news is that early fatty liver is often reversible. That is why doctors push for action early, before the liver moves from storage trouble to real injury.
Why this condition is often silent at first
Many young people feel completely fine when fatty liver first develops. There may be no pain, no obvious change in energy, and no warning sign that feels urgent enough to chase. According to Mayo Clinic’s MASLD overview, the condition often has no symptoms in its early stages.
That silence is part of the problem. Without symptoms, people usually do not ask for testing, and doctors may not find it until a routine blood test or scan shows a clue.
A quiet start can delay care in a few common ways:
- Testing gets skipped because the person feels normal.
- Diagnosis comes late because routine checkups miss it.
- Lifestyle changes wait until the problem is more advanced.
Silent fatty liver is easy to overlook, but it still can progress in the background.
That is why doctors are concerned. When a condition can sit unnoticed for years, it has more time to move from simple fat buildup to inflammation and scarring.
The biggest reasons more young people are getting fatty liver
Young adults are getting fatty liver for the same reason many chronic health problems start early: daily habits stack up over time. Diet, movement, sleep, stress, and blood sugar control all play a part, and they often feed into each other. A U.S. trend study of adolescents and young adults found that fatty liver prevalence rose sharply over time, especially in the 18 to 24 age group, which matches what many doctors are seeing now. See the U.S. trend study on young adults for the data behind that rise.
Fatty liver in young people usually comes from a mix of habits and metabolic strain, not one single mistake.
More ultra-processed food and sugary drinks

A diet heavy in added sugar, refined carbs, fast food, and processed snacks pushes the liver to store more fat. White bread, pastries, chips, candy, and fried takeout may feel harmless in the moment, but they add a lot of calories with very little fiber or staying power. When the body gets more sugar and starch than it can use, the liver helps turn that extra fuel into fat.
Sugary drinks are one of the biggest drivers because they flood the body fast. Soda, sweet tea, energy drinks, and many coffee drinks deliver a big sugar hit without making you feel full, so it’s easy to drink far more than you realize. That matters because liquid sugar skips the normal brakes that help control appetite.
Fast food and packaged snacks also make it easier to overeat. They are easy to grab, easy to finish, and often built to keep you coming back for more. Over time, that pattern can set the stage for liver fat, weight gain, and poor blood sugar control.
Less movement and more sitting time

Young people are also moving less during the day. School, office jobs, long commutes, homework, and hours on phones all add up to more sitting and less muscle use. When you sit for long stretches, your body burns less energy, and that makes weight gain more likely.
Less movement also affects how the body handles sugar. Muscles help pull glucose out of the blood, so regular activity makes blood sugar easier to manage. Without that movement, the body can become less responsive to insulin, which raises the chance of insulin resistance and liver fat buildup.
Small habits matter here. A long afternoon of scrolling, gaming, studying, or working at a desk can be enough to keep your body in a low-burn pattern all day. That is why a daily walking routine helps more than people think. Even short walks after meals can support better blood sugar control and reduce the strain on the liver.
Rising obesity, insulin resistance, and early diabetes
Excess body fat, especially around the waist, puts more pressure on the liver. Fat tissue is not just stored energy, it also affects hormones and inflammation. As a result, the liver gets a steady stream of fatty acids and more fat starts to collect inside liver cells.
This is why fatty liver often shows up with other metabolic problems. Insulin resistance, type 2 diabetes, high triglycerides, and high cholesterol all tend to travel together. When insulin stops working well, blood sugar rises, the body stores more fat, and the liver takes part of the hit. Then the cycle continues.
Many young people do not think of fatty liver as part of metabolic health, but it is. If weight gain, rising blood sugar, and abnormal lipids are already in the picture, the liver is often under strain too. That is why doctors look at the whole pattern, not just one lab value.
Common red flags that often show up together include:
- Abdominal weight gain, especially around the midsection
- Prediabetes or early diabetes
- High triglycerides
- Low HDL or high LDL cholesterol
- Fatigue after meals or unstable energy
When these issues overlap, the liver is often one of the first organs to show stress.
Sleep loss, stress, and poor routines
Short sleep and irregular schedules make healthy choices harder. If you stay up late, sleep in patches, or switch between work and school hours, hunger hormones and blood sugar control can get thrown off. Then cravings rise, energy drops, and it gets easier to reach for quick food instead of balanced meals.
Stress adds another layer. Many young adults eat for comfort when deadlines, money worries, or family pressure pile up. That can mean more snacks, more late-night eating, and more sugary drinks to keep going. Constant fatigue can also make exercise feel out of reach, so the cycle keeps building.
Better routines help more than people expect. A steadier bedtime, less late-night eating, and a few screen breaks during the evening can improve sleep quality and cut down on stress eating. If sleep is a weak spot, simple ways to fall asleep faster can make it easier to get back on track.
When sleep, stress, and food habits all slide at once, metabolic health usually follows. That is why fatty liver in young people is rarely about one habit alone. It is usually the result of several small pressures piling up at the same time.
Why today’s environment makes the problem worse
Young adults are not dealing with fatty liver in a vacuum. Their choices are shaped by a world built for speed, convenience, and constant stimulation, and that makes healthy routines harder to hold onto. Cheap calories are easy to find, movement gets squeezed out, and stress sits in the background all day.
That matters because fatty liver risk grows when the same pressures show up again and again. A person does not need a perfect diet or perfect routine to stay well, but modern life makes the unhealthy path much easier to repeat.
Food marketing, cheap calories, and easy access to junk food
Fast food, packaged snacks, and sweet drinks are everywhere. They are cheap, fast, and hard to ignore, especially for teens and young adults who are already busy, tired, or on a budget. A soda and fries can cost less than a balanced meal, which makes the shortcut feel normal.
Marketing also pushes these foods into daily life. Unhealthy food ads shape what people crave and buy, and that effect is strongest in younger groups. A recent narrative review on food marketing found that exposure to unhealthy ads is linked to higher intake of the advertised foods, which helps explain why these habits stick so easily unhealthy food marketing review.
When junk food is cheap, visible, and constantly promoted, it stops feeling like a treat and starts feeling like a routine.
That routine matters for the liver. Sugary drinks, fried takeout, and salty packaged snacks add calories fast, but they do not keep you full for long. If you want the bigger picture on habit change, this guide on how to build better eating habits fits the same problem.
More screen time and fewer natural movement breaks
Phones, gaming, streaming, and remote work have changed how people spend their day. You can go hours without standing up and barely notice it. A student can attend class, scroll between assignments, and order food without taking more than a few steps.
That is different from how daily movement used to happen. People walked to class, stood in lines, ran errands, cleaned more by hand, and moved through the day in smaller bursts. Those built-in breaks added up.
Screen time also changes what happens around food. It often leads to distracted eating, later bedtimes, and less exercise. In college-aged adults, leisure screen time has been linked with higher BMI, larger waist size, and worse cardiometabolic markers, which helps explain why sitting time matters so much screen time and cardiometabolic health.
A few missed steps do not sound serious. Still, when they happen every day, they lower energy use, weaken blood sugar control, and make fat gain more likely. That is one reason so many young adults drift into a sedentary pattern without ever planning to.
Some medications and medical conditions can add risk
Certain medicines and health issues can raise fatty liver risk, but they are usually part of a larger metabolic picture. Conditions like insulin resistance, type 2 diabetes, high triglycerides, obesity, and sleep apnea matter much more often than rare causes do. Mayo Clinic lists several of these common linked conditions, along with less common contributors such as hypothyroidism and polycystic ovary syndrome Mayo Clinic on MASLD causes.
Some medications can also contribute in certain people, especially when other risk factors are already present. That includes a few drugs used for cancer, autoimmune disease, or seizure disorders. Even then, the medication usually adds to the problem instead of creating it alone.
The main point is simple. Most young adults with fatty liver are dealing with a mix of diet, inactivity, weight gain, and insulin resistance. Medications and medical conditions can nudge that risk higher, but they rarely explain the full picture on their own.
How fatty liver in young people can be spotted earlier
Fatty liver often stays hidden until a routine exam finds a clue. That is why early screening matters, especially for young adults who already have metabolic risk. Damage can build for years before anyone feels sick, so waiting for symptoms can mean waiting too long.
Doctors usually look for patterns, not one isolated sign.
Common clues doctors check for

A few findings can raise suspicion, especially when they show up together. Belly weight gain, abnormal liver tests, high blood sugar, high triglycerides, and a family history of metabolic disease all point in the same direction. None of these confirms fatty liver on its own, but they can tell a doctor to look closer.
Common clues include:
- Waist or belly gain, especially with little change in overall health
- Abnormal liver tests, such as a higher-than-expected ALT
- High blood sugar or prediabetes
- High triglycerides or other lipid problems
- Family history of type 2 diabetes, obesity, or metabolic syndrome
A normal routine day can hide a liver problem for years, but a pattern of small clues often shows up first.
Why blood tests and imaging may be needed
Blood tests help, but they do not tell the full story. Liver enzymes can be high, yet they can also look normal even when fat is already present in the liver. That is why doctors often combine lab work with imaging or other tests, especially in people with obesity, diabetes, or other cardiometabolic risks.
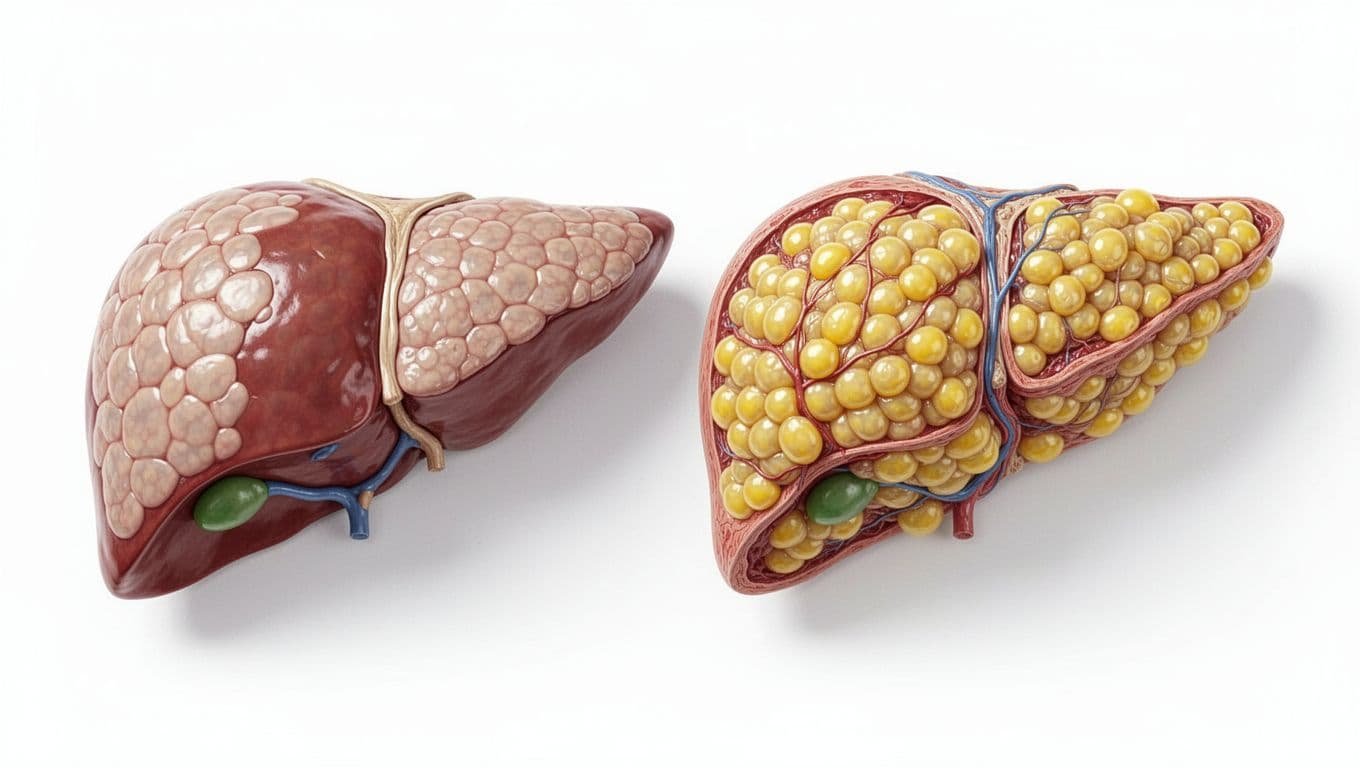
Ultrasound can show fat in the liver, while elastography can check liver stiffness, which helps suggest scarring. Some doctors also use blood-based fibrosis scores to decide who needs a closer look, and current MASLD management guidelines support a step-by-step approach in higher-risk people.
A simple way to think about it: blood tests can raise the alarm, but imaging often shows what the alarm is pointing to.
Who should ask about screening sooner
People with obesity, type 2 diabetes, high cholesterol, or a strong family history should bring up screening earlier, even if they feel fine. If you already track blood sugar or lipids, ask whether liver tests should be part of that same checkup.
That matters because fatty liver often travels with other metabolic issues. When one risk factor is already there, the liver may be under strain too. If high cholesterol is part of your picture, diet changes that lower LDL can support the same overall risk profile doctors watch during screening.
The safest move is simple, ask early, especially if your weight, blood sugar, or cholesterol has changed over time. Early detection gives you more room to reverse the trend before scarring becomes harder to stop.
What young adults can do now to lower their risk
The good news is that fatty liver risk is not fixed. Small changes in food, movement, and follow-up care can lower the strain on your liver, even if your schedule is packed. You do not need a perfect routine, you need a better pattern that you can keep.
A few steady habits can lower liver fat and improve how your body handles sugar. That matters because the liver responds to what you do most days, not just what you do once in a while.
Early changes can make a real difference, especially before liver damage has time to build.
Simple food swaps that help the liver

Start with swaps that fit real life. Replacing sugary drinks with water, sparkling water, or unsweetened tea cuts a big source of extra sugar without making meals feel complicated. That one change alone can take pressure off the liver.
You can also choose less processed food more often. Frozen vegetables, canned beans, plain oats, eggs, tuna, Greek yogurt, and brown rice are usually affordable and easy to build around. For more guidance on diet patterns that support liver health, Mayo Clinic’s MASLD diet advice gives a practical starting point.
A simple plate works well:
- More fiber from vegetables, beans, oats, and fruit
- More protein from eggs, fish, yogurt, chicken, tofu, or beans
- Less added sugar from soda, candy, pastries, and sweet coffee drinks
If money is tight, build meals around what stretches. A bag of frozen vegetables, a rotisserie chicken, and a pot of rice can cover several meals. The goal is not perfection, it is making the next meal a little better than the last.
Movement goals that fit real life

Daily movement helps the body use sugar better, which can reduce fat stored in the liver. Regular walking is a strong place to start, especially if you are not exercising now. Even a 10-minute walk after meals can help.
Strength training matters too. Bodyweight squats, push-ups, resistance bands, and dumbbells all help build muscle, and muscle improves blood sugar control. You do not need a gym membership to begin.
Long sitting periods also matter. If you study or work at a desk, stand up, stretch, or walk for a few minutes each hour. That small break keeps your body from settling into a low-movement routine all day.
A realistic weekly target looks like this:
- Walk most days, even if the walk is short.
- Add two or three strength sessions each week.
- Break up long sitting with brief movement breaks.
For young adults trying to build a simple routine, how to reduce belly fat fast includes habits that pair well with liver-friendly movement.
When lifestyle changes are not enough on their own
Some people need medical support, especially if they already have diabetes, obesity, high cholesterol, or signs of liver damage. In those cases, diet and exercise still matter, but they may not be enough by themselves.
Seeing a doctor early is better than waiting for symptoms. Fatty liver often stays quiet, so waiting until you feel sick can mean waiting until the problem has moved further along. A doctor can check blood sugar, lipids, liver tests, and whether imaging makes sense. Current MASLD guidelines also support earlier case-finding in people with higher metabolic risk.
If your labs are off or your weight has climbed, bring it up now. Early care gives you more options, and in many young adults, it gives the liver a real chance to bounce back.
Conclusion
More young people are developing fatty liver because the same pressures keep showing up earlier in life: more ultra-processed food, less daily movement, and more signs of metabolic strain like insulin resistance and weight gain. That pattern explains why MASLD is now showing up in teens and young adults more often.
The main takeaway is simple, fatty liver can often be reversed early. When people catch it sooner and make steady changes in food, movement, sleep, and follow-up care, they give the liver a much better chance to recover before scarring starts.
That makes early screening and small daily habits worth taking seriously. A few better choices, repeated often, can protect liver health long before serious damage begins.
Sav pin for later
- Why Fiber Is the Standard for Your Home Internet - 16/05/2026
- How to Bounce Back From a Setback (A Step-by-Step Guide) - 16/05/2026
- 12 Practical Ways to Rebuild Your Confidence After Failure - 16/05/2026
