Your liver handles a heavy load every day, filtering sugar, fat, chemicals, and toxins from what you eat and drink. The trouble is that damage can build slowly, long before you feel sick.
Some foods look harmless, but eating them often can push the liver toward fatty liver, inflammation, and long-term stress. Sugary drinks, fried foods, refined carbs, and ultra-processed snacks are common examples, and the biggest risk is how often they show up in your routine.
The good news is that you can spot the pattern early and make smarter swaps before the damage adds up. If you want a useful starting point, liver cleansing foods can help balance out the foods you should watch first, and the sections below break down what matters most.
How food choices can quietly overload the liver
Your liver handles a lot of what you eat and drink, so meal after meal matters more than one bad choice. When your diet is heavy in fructose, added sugar, refined oils, and processed ingredients, the liver has to keep sorting, storing, and converting that load. Over time, that work can stack up fast.
A good place to start is reducing sugar for fatty liver health, because sugar is one of the easiest ways to push the liver past its comfort zone. A review in PubMed Central also links added fructose with fatty liver risk, which fits what happens in real life when sweet drinks and packaged foods become everyday habits.
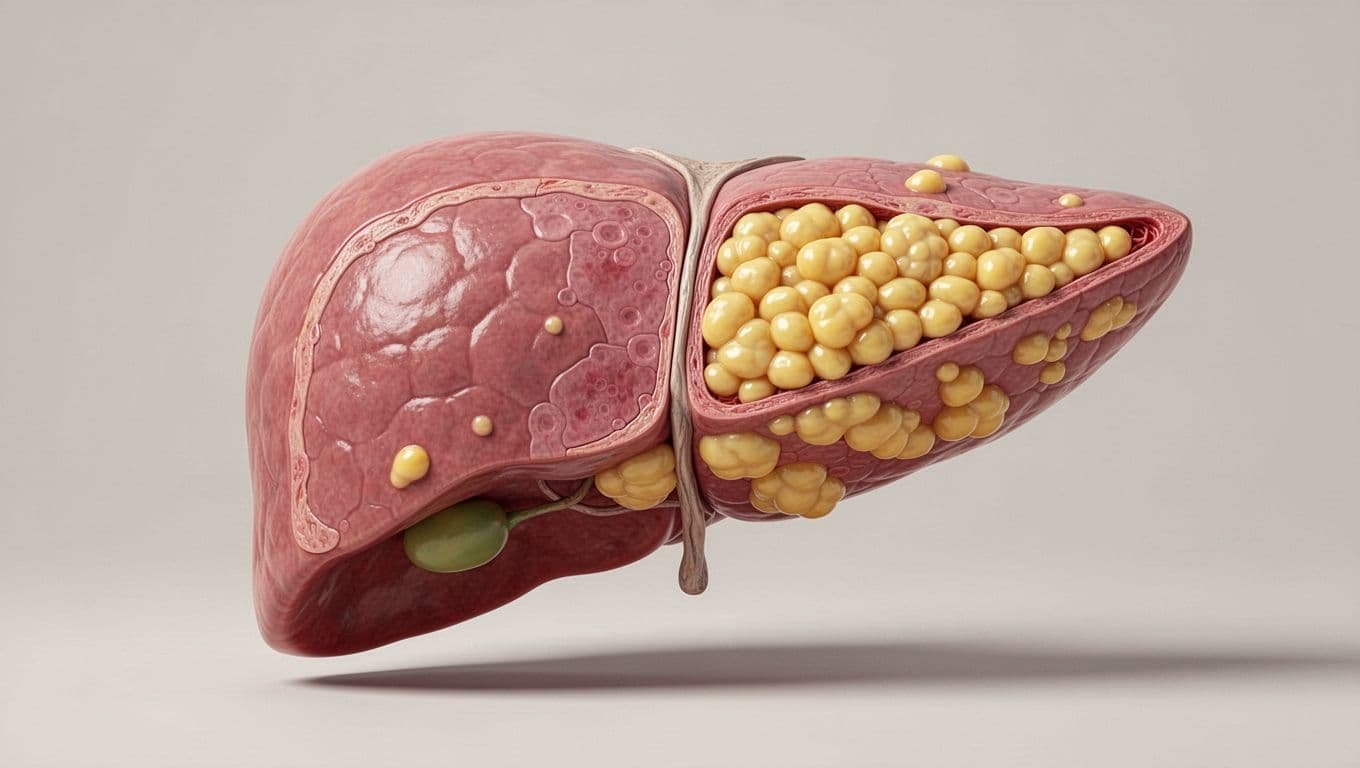
Why the liver takes the hit first
The liver is the body’s main processing hub for nutrients, alcohol, and many food byproducts. That means it gets first access to a lot of the sugar and fat you consume, especially fructose and alcohol-related compounds. When those show up often, the liver has less room to keep up.
In other words, a poor diet does not have to wreck the whole body at once. It often starts with the liver because the liver is doing the cleanup work.
What happens when fat and sugar build up over time
When you eat more sugar and fat than your body can use, the extra fuel gets stored inside liver cells. That is how fatty liver starts, in plain terms. The cells swell, the liver gets stressed, and its work slows down.
As the buildup continues, insulin resistance can set in, which makes it even easier for more fat to collect. That cycle also feeds inflammation, so the liver has to deal with both storage overload and irritation at the same time.
Sugary drinks are one of the biggest hidden threats
Sugary drinks are easy to miss because they feel harmless in the moment. A soda, sweet tea, fruit drink, flavored coffee, sports drink, or energy drink can add a big sugar load fast, and your liver has to deal with most of it.
That matters because liquid sugar often contains a lot of fructose. When intake gets high, the liver turns more of that sugar into fat, which can build up over time and raise the risk of fatty liver. A systematic review in PubMed found that fructose-containing sugar from sugar-sweetened drinks is tied to higher liver fat markers, which lines up with what many people see in everyday eating habits.

Why fructose is so hard on the liver
Fructose is processed mainly in the liver, so it gets a direct path there. When you drink a lot of it, the liver can turn the extra into fat rather than using it for energy.
Over time, that can push the liver toward fat buildup and inflammation. Soft drinks and sweetened beverages are a common source, which is why they show up so often in fatty liver discussions.
Why liquid calories are easier to overdo
Drinks do not fill you up the way food does. You can sip soda or sweet tea quickly, finish the bottle, and still feel ready for a meal.
That makes liquid sugar a problem. Your body gets the calories, but your brain misses the cue to stop. If you want a simple place to start, cut back on sugary drinks and watch what changes in your daily routine.
Better swaps that still taste good
Small swaps make a big difference here. You do not need a perfect diet to protect your liver.
Try these first:
- Water for the easiest no-sugar option
- Sparkling water when you want bubbles
- Unsweetened tea for flavor without the sugar hit
- Fruit-infused water with lemon, cucumber, or berries
These drinks keep the routine familiar without flooding the liver with sugar.
Processed snacks and breakfast foods can be sneakier than they look
Packaged cereals, pastries, cookies, granola bars, and flavored yogurts often wear a health halo they don’t deserve. They may look light or convenient, but many of them are built on refined flour, added sugar, and very little fiber. That mix can hit your bloodstream fast, then send more fat toward the liver over time.
A recent meta-analysis on ultra-processed foods and fatty liver risk found a clear link between higher ultra-processed food intake and NAFLD. That fits the pattern many people miss at breakfast, where the most convenient option is often the least liver-friendly.

Why fat-free does not always mean liver-friendly
Fat-free labels can sound healthy, but food makers usually replace fat with sugar, starch, or both to keep the taste appealing. That keeps the product easy to eat, yet it often makes it worse for the liver.
A fat-free flavored yogurt or cereal can still act like dessert in disguise. If it tastes sweet and goes down fast, your liver still has to deal with the sugar load.
How low fiber makes the problem worse
Fiber slows down how fast sugar enters your blood. Without it, blood sugar rises faster, insulin works harder, and the liver gets more pressure to store the extra energy as fat.
That is why a bowl of sugary cereal or a soft granola bar rarely keeps you full for long. If breakfast leaves you hungry soon after, it usually did not help your liver much either.
For a better start, choose meals with protein, fiber, and less added sugar, like the kinds of options covered in healthy breakfast ideas for busy mornings.
Fried foods and fast food can drive liver inflammation
Fried meals can hit the liver from several angles at once. The oil, the breading, and the extra calories all add up, so the damage is bigger than a single ingredient on its own.
When fries, fried chicken, onion rings, and fast-food burgers show up often, the liver gets stuck handling unhealthy fats, refined carbs, and excess energy together. That mix can raise inflammation, promote fat buildup, and make it harder for the liver to stay balanced.

The role of trans fats and reused oils
Deep-frying often damages the oil itself. When oils are heated again and again, they form oxidized compounds that raise oxidative stress, which is a direct strain on your cells. Research also links fried oils and trans fats with liver fat buildup and inflammation, especially when these foods are eaten often.1
Trans fats are especially hard on the body because they change how fats are processed and stored. Reused oils can do the same thing, since they expose the liver to broken-down fats that are harder to manage.
Why fast food is more than just high in calories
Fast food usually stacks several problem foods in one meal. A burger, fries, and a soda can combine refined flour, sugar, salt, and poor-quality fats in a way that gives the liver a heavy load.
Common examples include:
- Fries and onion rings, which bring starch and fried oil together
- Fried chicken, which adds breading plus absorbed fat
- Fast-food burgers, which often include refined buns, fatty meat, and salty sauces
A recent review of ultra-processed foods found higher intake was linked with greater fatty liver risk, which matches the pattern seen with frequent fast-food meals.2
Healthier cooking methods that still feel satisfying
You don’t have to give up flavor to ease the strain on your liver. Better methods can still give you crisp edges, rich taste, and a filling meal.
Try these options more often:
- Baking for chicken, potatoes, and fish
- Grilling for burgers, vegetables, and lean meats
- Roasting for a browned, savory finish
- Air-frying for a crunchy texture with less oil
- Using smaller amounts of better-quality oils like olive oil

These swaps keep meals satisfying while cutting back on the fried-food load that pushes the liver toward inflammation.
Red meat, bacon, and deli meats can add pressure to the liver
Red meat can fit into a balanced diet, but frequent large servings of bacon, sausage, hot dogs, and deli meats create a different pattern. These foods often bring more saturated fat, sodium, and preservatives than fresh cuts, and that mix can add extra work for the liver over time.
A 2024 systematic review and dose-response meta-analysis found a link between red meat, processed red meat, and a higher risk of nonalcoholic fatty liver disease. Processed meats are the bigger concern because they are usually eaten in larger daily portions and come with additives such as nitrates or nitrites. That does not mean one slice of bacon ruins anything, but daily use can turn a small habit into a steady burden.

Why processed meats are a bigger concern than fresh cuts
Fresh beef, pork, or lamb still contain saturated fat, but processed meats usually stack on more risk. Bacon, sausage, hot dogs, and deli meats often have higher sodium, plus preservatives that help them last longer on the shelf.
That matters because high sodium can strain blood pressure and water balance, while processed additives can add to the liver’s load. In plain terms, fresh meat is a simpler ingredient list, and that usually makes it easier to manage in everyday meals.
Better protein choices for everyday meals
You can still eat well without relying on processed meats. Fish, chicken, beans, lentils, tofu, and other lean or plant-based proteins are easier choices for most days.
A simple rule helps: use red meat as an occasional food, not a daily staple. For more meal ideas that fit that pattern, try healthy protein-packed dinners for busy nights. When you build meals around lighter proteins, the liver gets less saturated fat and fewer additives to process.
Ultra-processed meals can damage the liver from more than one angle
Ultra-processed meals are a problem because they rarely hit the liver in just one way. Packaged frozen meals, instant noodles, chips, boxed dinners, and drive-thru meals often combine refined carbs, unhealthy fats, added sugar, and high sodium in the same package. That mix can push fat storage, raise inflammation, and make the liver work harder after every meal.

A recent review in Frontiers in Nutrition found that higher ultra-processed food intake is linked with greater NAFLD risk. That fits what happens in real life, since these meals are built for convenience, not liver support.
Why ingredient lists matter as much as calories
A low calorie count can hide a messy label. If you see a long ingredient list with added sugars, refined oils, starches, flavor enhancers, and preservatives, the food is usually doing more than simply filling you up.
Calories matter, but they don’t tell the whole story. Two meals can look similar on paper, yet one may be far easier on your liver because it uses simpler ingredients and less added sugar.
The gut-liver connection in simple terms
Your gut and liver talk to each other all day. When ultra-processed foods crowd out fiber and whole foods, gut health can slip, and more unwanted compounds can pass through the intestinal barrier.
That extra load can reach the liver through the portal vein, where it adds to the liver’s cleanup work. Over time, that can mean more irritation, more inflammation signals, and more strain than your body needs. In plain terms, a stressed gut often sends a stressed liver even more to handle.
Energy drinks and alcohol-like stress without the alcohol
Energy drinks can put the liver under pressure in a way that feels a lot like alcohol-related strain, even when no alcohol is involved. The problem is the formula itself, which often combines high caffeine, a large sugar load, artificial sweeteners, taurine, niacin, and other additives in one can.

Why caffeine and sugar together can be a bad mix
Caffeine can make you feel alert, while sugar gives a fast lift, so the combo makes it easy to overdo it. That matters because energy drinks can add extra calories fast, and the liver often turns excess sugar into fat when intake is frequent.
Over time, that pattern can raise liver strain, especially if energy drinks replace meals or get added on top of an already high-sugar diet. The NIH LiverTox review on energy drinks notes that excess use has been linked to acute liver injury in some cases, which is a reminder that “energy” can come with a cost.
When a quick boost becomes a daily habit
A single can before work or class can turn into a routine before you notice it. That habit adds up, especially when the drink becomes the answer to poor sleep, long hours, or skipped meals.
People with weight gain, insulin resistance, or other metabolic issues may feel the impact sooner, since their liver already has more to manage. Frequent use can also mask fatigue instead of fixing it, which keeps the cycle going. If you need a safer pattern, start by cutting back on the days you use them most and watch how your energy changes without the crash.
Foods That Carry Toxins or Contamination Can Harm the Liver Too
Some foods cause liver stress even when the recipe itself looks harmless. The problem is contamination, not the label on the package. Mold, poor storage, and bad sourcing can bring in toxins that the liver has to filter out.
That matters most with staple foods like grains, peanuts, corn, and nuts. If they sit in warm, damp places, they can develop toxins that build up risk over time.

How mold toxins affect the liver
Aflatoxins are one of the biggest concerns because they target the liver directly. The National Cancer Institute notes that aflatoxins are found on crops like corn, peanuts, cottonseed, and tree nuts, and long-term exposure is tied to higher liver cancer risk.
That risk matters because aflatoxins can damage the liver in two ways. High exposure can injure it fast, while lower exposure can add up over time. Foods with visible mold are an obvious warning, but the bigger issue is that some contamination is hidden.
Easy storage and shopping habits that reduce risk
Simple habits lower the chance of bringing these toxins home. Buy grains, nuts, and peanut products from trusted sources, check freshness dates, and avoid packages that look damaged or stale. Also, store dry foods in cool, dry places, because heat and moisture help mold grow.
A few smart habits go a long way:
- Choose sealed packages from reliable stores
- Check for off smells, clumping, or discoloration
- Keep pantry foods dry and cool
- Throw out anything moldy or rancid
If you want to protect your liver, sourcing and storage matter just as much as the food itself.
Conclusion
The biggest liver risks often hide in plain sight, especially sugary drinks, ultra-processed foods, fried meals, processed meats, and contaminated foods. Those habits can add sugar, bad fats, sodium, and toxins faster than most people realize, which is why the damage builds slowly.
The good news is that your liver can handle a lot when the pressure eases. Small daily changes matter, so choose whole foods more often, drink fewer sugary beverages, read labels with care, and cook at home when you can. Those simple choices give your liver less to process and more room to do its job well.
Footnotes
Save pin for later

- Why Fiber Is the Standard for Your Home Internet - 16/05/2026
- How to Bounce Back From a Setback (A Step-by-Step Guide) - 16/05/2026
- 12 Practical Ways to Rebuild Your Confidence After Failure - 16/05/2026
